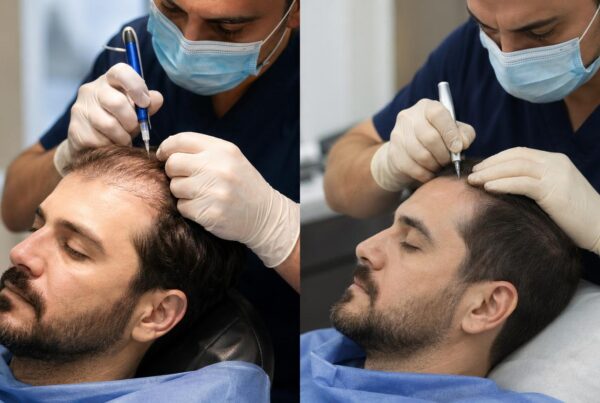
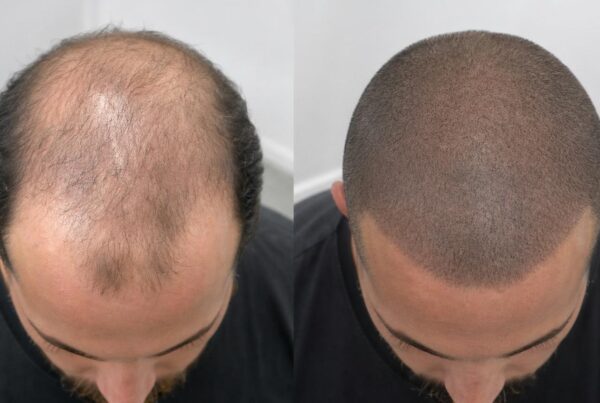
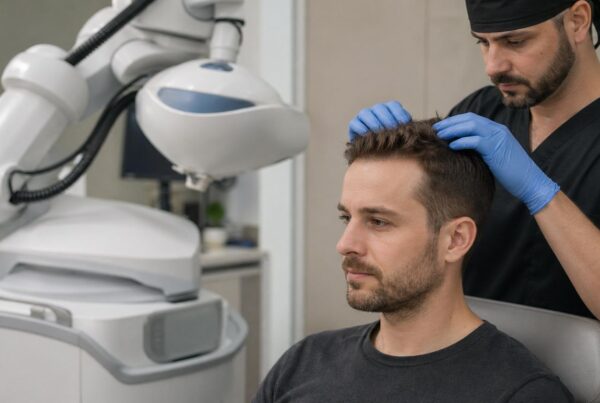
One of the most common questions patients ask after booking their procedure is when it’s safe to drink alcohol after a hair transplant. The answer is more nuanced than a single date on the calendar, because alcohol affects nearly every biological process involved in graft healing: blood clotting, tissue hydration, nutrient delivery, and medication metabolism. Research published in the Journal of Clinical and Aesthetic Dermatology confirms that alcohol consumption within the perioperative window significantly increases complication rates for follicular procedures. Surgeons at leading clinics in Istanbul, including the team at Estenove, consistently advise patients to plan their social calendars carefully around the procedure. The stakes are real: each transplanted graft represents a one-time investment, and a single night of heavy drinking can compromise months of planning. This guide breaks down the exact timeline, the biological reasons behind the restriction, and a practical framework for reintroducing alcohol without jeopardizing your results.
The Recommended Hair Transplant Alcohol Timeline
A clear, evidence-based timeline removes guesswork. Most board-certified surgeons follow a similar protocol, though slight variations exist depending on the technique used (FUE, DHI, or stem cell-assisted transplant) and the patient’s individual health profile. The general framework looks like this:
- 7 days before surgery: Stop all alcohol consumption entirely.
- Day 0 (surgery day): Absolute zero alcohol in your system.
- Days 1-7 post-op: Strict abstinence during the critical graft stabilization phase.
- Days 7-14 post-op: Continued abstinence recommended; grafts are still anchoring into the scalp’s blood supply.
- Day 14+ post-op: Light, moderate consumption may be reintroduced with your surgeon’s approval.
- Day 30+ post-op: Most patients can return to normal social drinking patterns.
This timeline is not arbitrary. Each phase corresponds to a specific stage of wound healing and graft vascularization that alcohol directly interferes with.
Why You Must Avoid Drinking Before Surgery
The pre-operative window matters just as much as the post-operative one. Alcohol remains active in your bloodstream for 24-72 hours depending on the quantity consumed, and its anticoagulant effects persist even after you feel sober. According to Dr. Robert Leonard, a hair restoration surgeon with over 30 years of clinical experience, even two glasses of wine the night before surgery can measurably increase intraoperative bleeding.
Excessive bleeding during an FUE or DHI procedure creates several problems. The surgeon’s visibility is reduced, making precise graft extraction and placement more difficult. Blood pooling around recipient micro-channels can physically dislodge freshly placed follicles. The anesthetic solution, which contains epinephrine to control bleeding, becomes less effective when competing against alcohol’s vasodilatory effects. Stopping alcohol a full seven days before surgery gives your liver time to fully metabolize residual ethanol and allows platelet function to normalize.
The Critical Waiting Period After Your Procedure
The first 10 days after your transplant represent the highest-risk window. During this phase, each transplanted follicular unit is held in place only by a tiny blood clot and the surrounding tissue’s inflammatory response: a fragile anchor at best. Full vascularization, where new blood vessels grow into the transplanted follicle, typically takes 7-10 days.
Drinking during this window introduces two simultaneous threats. First, alcohol thins the blood and destabilizes the clots holding grafts in place. Second, it triggers vasodilation (widening of blood vessels), which increases swelling and pressure in the scalp. Surgeons report that patients who drink within the first week are significantly more likely to experience graft displacement, prolonged redness, and poor initial healing. The safest approach is to treat the first two weeks as a strict no-alcohol zone, no exceptions.
How Alcohol Impacts Graft Survival and Recovery
Understanding the biology helps explain why surgeons are so firm about this restriction. Graft survival is not guaranteed simply because follicles were placed correctly during surgery. The post-operative environment determines whether those follicles establish a permanent blood supply or die.
Alcohol as a Blood Thinner and Risk of Hemorrhage
Ethanol inhibits platelet aggregation, which is the body’s primary mechanism for forming blood clots. A 2019 study in Thrombosis Research found that even moderate alcohol intake (two standard drinks) reduced platelet aggregation by 15-25% for up to 48 hours. For a hair transplant patient with 3,000-4,000 micro-wounds on their scalp, this is significant.
Each recipient site is essentially a tiny incision, typically 0.7mm to 1.0mm in diameter. These sites rely on rapid clot formation to hold the graft in place and seal the wound. When clotting is impaired, patients may notice pinpoint bleeding from recipient sites, blood-stained pillows in the morning, or visible oozing when they gently touch the transplant area. In severe cases, grafts can be lost entirely. The hemorrhage risk is highest in the first 72 hours but remains elevated for the full first week.
Dehydration and Impaired Nutrient Flow to New Grafts
Alcohol is a potent diuretic. It suppresses antidiuretic hormone (ADH), causing your kidneys to excrete more water than you’re taking in. This creates a state of systemic dehydration that directly affects the scalp’s microcirculation.
Transplanted follicles depend on plasma-rich blood flow to deliver oxygen, glucose, and growth factors to the healing tissue. Dehydrated blood is thicker, moves more slowly through capillaries, and carries fewer dissolved nutrients. The result is a hostile environment for new grafts trying to establish vascular connections. Clinical observations suggest that well-hydrated patients (consuming 2.5-3 liters of water daily post-op) show faster healing and better graft take rates compared to those who are even mildly dehydrated.
Potential Interactions with Post-Op Medications
Most hair transplant patients are prescribed a post-operative medication regimen that typically includes antibiotics (often cephalexin or azithromycin), anti-inflammatory drugs, pain relievers, and sometimes minoxidil or finasteride. Alcohol interacts negatively with nearly all of these.
Mixing alcohol with antibiotics can reduce their effectiveness and increase the risk of gastrointestinal side effects like nausea and vomiting. Combining alcohol with pain medications, particularly acetaminophen-based drugs, places enormous strain on the liver: the combination is one of the leading causes of acute liver injury in otherwise healthy adults. Anti-inflammatory medications like ibuprofen already carry a bleeding risk, and alcohol amplifies this significantly. Even minoxidil, a topical vasodilator, can cause exaggerated drops in blood pressure when combined with alcohol’s own vasodilatory effects. The safest rule is simple: do not drink while taking any post-operative medication.
Best Practices for Resuming Alcohol Safely
Once your surgeon clears you, typically around the two-week mark, reintroduction should be gradual and deliberate. Your body has been through a medical procedure, and your scalp is still in an active healing phase that continues for several months.
Starting with Moderate Consumption
Begin with a single glass of wine or one beer, not a full night out. Monitor how your scalp responds over the next 24 hours. Look for increased redness, swelling, or any sensation of throbbing in the recipient area. If none of these occur, you can gradually return to your normal patterns over the following two weeks.
Avoid spirits with high alcohol concentrations (40%+) during the first month, as these cause more pronounced vasodilation and dehydration per serving. Red wine, while often cited for its antioxidant content, is also higher in histamines and can trigger scalp inflammation in sensitive individuals. Light beer or a single glass of white wine is the most conservative starting point.
Prioritizing Hydration to Protect Hair Health
For every alcoholic drink you consume in the first three months post-transplant, match it with at least two full glasses of water (approximately 500ml). This counteracts alcohol’s diuretic effect and helps maintain the plasma volume your healing follicles need.
Consider adding an electrolyte supplement to your water, particularly one containing potassium and magnesium, which alcohol depletes rapidly. Track your daily water intake using a simple app or marked water bottle. Aim for a minimum of 2.5 liters on days you consume any alcohol. This single habit can meaningfully protect the microcirculation that feeds your new grafts during the critical growth phase between months one and four.
FAQ
Most surgeons consider light drinking acceptable after 14 days, provided your healing is on track and you’ve completed your antibiotic course. Start with one drink and observe your scalp’s response before increasing.
Alcohol inhibits platelet aggregation by 15-25%, impairing your blood’s ability to form stable clots. Since each transplanted graft sits in a micro-wound roughly 0.7-1.0mm wide, weakened clotting can lead to graft displacement and prolonged bleeding.
A single drink after the two-week mark is unlikely to cause measurable damage. However, one drink within the first 72 hours post-surgery could genuinely compromise graft survival due to the fragile state of healing tissue.
Yes. Alcohol reduces clotting, dehydrates tissue, impairs nutrient delivery, and interacts with post-operative medications: all of which directly threaten graft take rates during the first two weeks.
The minimum recommended abstinence period is 14 days post-surgery, with 7 days of pre-operative abstinence as well. For the best possible results, many surgeons recommend a full 30 days of post-operative sobriety.