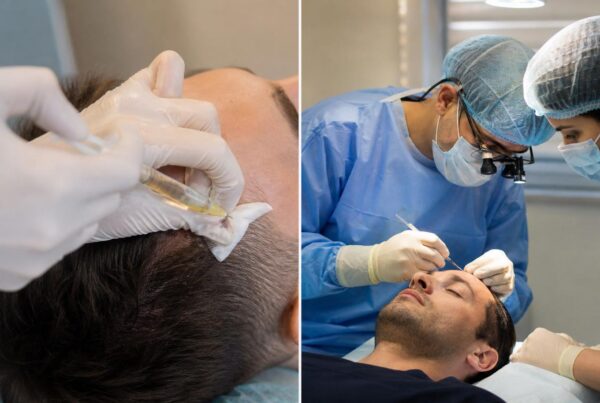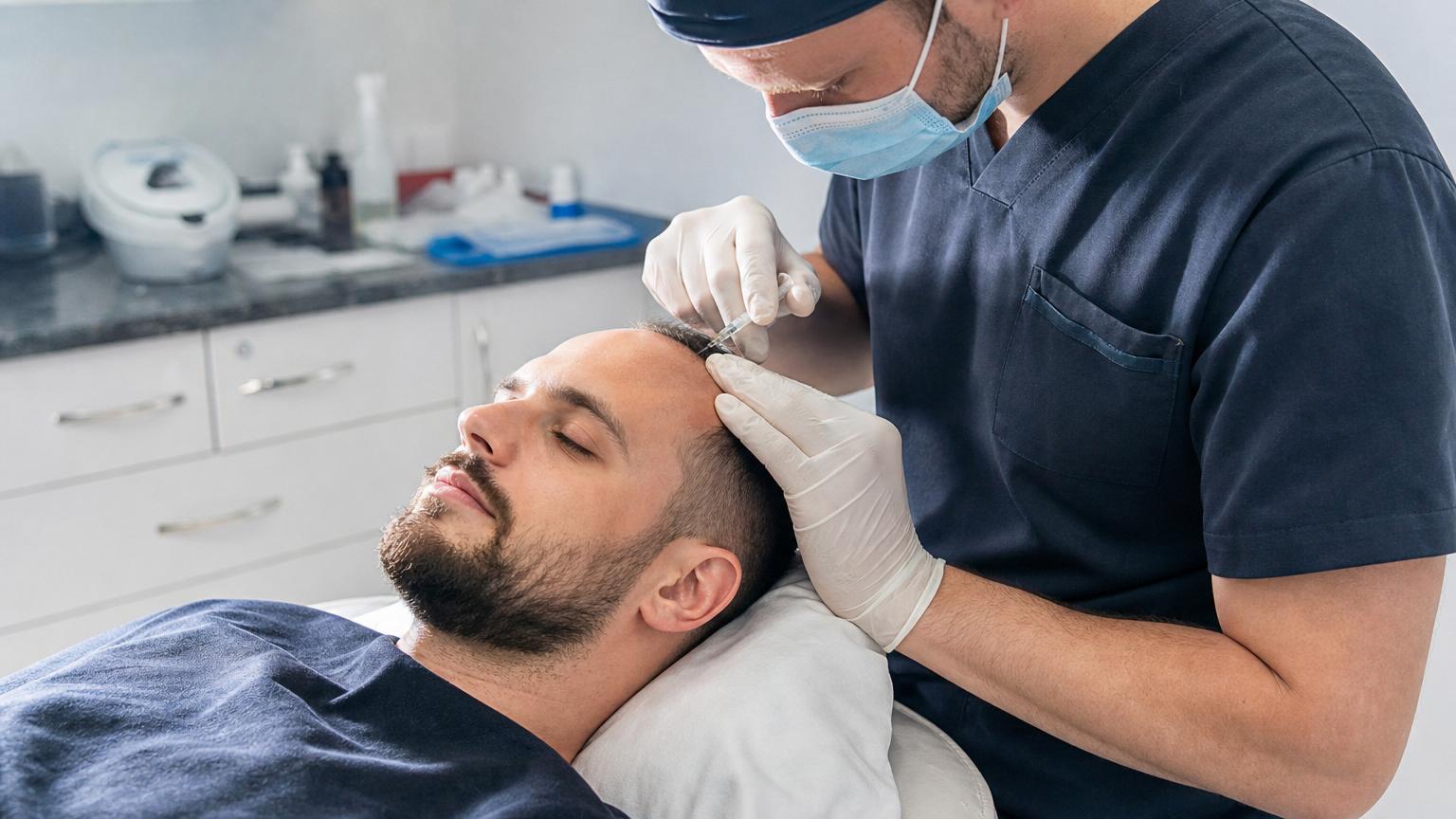
One of the most common questions prospective patients ask before booking a procedure is whether a hair transplant process is painful. The honest answer is that modern anaesthesia protocols have made the experience far more comfortable than most people expect. A 2022 survey published in the Journal of Cosmetic Dermatology found that 87% of hair transplant patients rated their intraoperative pain as 3 or below on a 10-point scale. That statistic reflects genuine advances in how clinics administer local anaesthesia, manage anxiety, and control post-operative discomfort. Fear of pain remains the single biggest barrier to booking a procedure, yet the reality rarely matches the expectation. This guide breaks down exactly what you will feel at each stage, what anaesthesia techniques are used, and how to manage recovery with minimal discomfort.
Understanding Hair Transplant Pain and Patient Experience
Pain perception during a hair transplant depends on several variables: the technique used, the surgeon’s skill, the patient’s individual pain threshold, and the quality of the anaesthesia protocol. Most discomfort is concentrated in the first few minutes of the procedure, specifically during the initial anaesthetic injections into the scalp. Once the local anaesthesia takes full effect, typically within 10 to 15 minutes, the donor and recipient areas become completely numb. Patients often describe the sensation during graft extraction and implantation as mild pressure or a tugging feeling, not pain.
Anxiety amplifies the perception of discomfort. Clinics that invest in pre-operative counselling and a calm environment consistently report lower patient pain scores. Understanding the timeline of sensations helps set realistic expectations and reduces the fear that causes many people to delay treatment for years.
Common Sources of Hair Transplant Discomfort
The primary sources of hair transplant discomfort are the anaesthetic injections themselves, prolonged sitting in the surgical chair, and post-operative tightness in the donor area. The scalp has a dense network of nerve endings, so the initial needle pricks can sting. Most patients compare it to a dental injection: brief, sharp, and quickly forgotten once numbness sets in.
Sitting for 6 to 10 hours can cause neck stiffness and lower back ache. Clinics that offer ergonomic chairs, periodic stretch breaks, and neck support pillows reduce this significantly. After surgery, the donor area may feel tight or sore for 48 to 72 hours, particularly with strip-based methods where a linear incision is involved.
FUE vs. FUT: Pain Levels During and After Surgery
Follicular Unit Extraction (FUE) and Follicular Unit Transplantation (FUT) differ meaningfully in their pain profiles. FUE uses a micro-punch tool, typically 0.7mm to 1.0mm in diameter, to extract individual follicular units. Because there is no linear incision, post-operative pain is generally mild, and most patients report discomfort levels of 2 to 3 out of 10 during recovery.
FUT involves removing a strip of scalp tissue from the donor area, which is then sutured closed. This creates a more significant wound, and patients typically report higher pain scores of 4 to 6 out of 10 during the first 72 hours. FUT also carries a longer healing timeline: sutures are removed at 10 to 14 days, and the incision site can feel tight for several weeks. For patients prioritizing minimal pain during a hair transplant, FUE is the clear choice.
The Hair Transplant Anaesthesia Guide
A well-executed anaesthesia protocol is the single most important factor in determining whether a patient has a comfortable experience. The vast majority of hair transplants worldwide are performed under local anaesthesia, meaning the patient remains fully awake while the scalp is completely numbed. General anaesthesia is almost never necessary and introduces unnecessary risk.
Local Anaesthesia Techniques for a Numb Scalp
Surgeons typically use a combination of lidocaine (1% or 2%) with epinephrine to achieve full scalp numbness. The epinephrine constricts blood vessels, which reduces bleeding and extends the duration of the anaesthetic effect. A ring block technique is common: the surgeon injects anaesthetic around the perimeter of the donor area and recipient zone, creating a complete field of numbness.
The initial injection uses a fine 30-gauge needle inserted to a depth of approximately 0.5mm to 1.5mm into the subcutaneous tissue. After the first few injections take hold, subsequent ones are placed into already-numb tissue, so the patient feels progressively less. Top-up doses are administered every 2 to 3 hours throughout longer procedures to maintain full numbness. According to Dr. John Cole, a respected transplant surgeon, properly administered local anaesthesia should make the entire procedure virtually painless after the first five minutes.
Modern Painless Injection Systems
Several clinics now use needle-free injection systems that deliver anaesthetic through high-pressure air rather than a traditional needle. These devices, such as the Comfort-In system, force a fine jet of lidocaine through the skin at pressures of around 3,000 PSI. Patients typically describe the sensation as a brief snap rather than a sting, and studies show a 70% reduction in injection-related pain scores compared to conventional needles.
Some clinics, including Estenove in Istanbul, combine needle-free systems with vibration anaesthesia devices that stimulate surrounding nerve fibres and block pain signals during the initial injections. Pre-treatment with a topical anaesthetic cream containing 2.5% lidocaine and 2.5% prilocaine, applied 30 to 45 minutes before the procedure, further reduces sensation at the injection sites.
Managing Pain During Hair Transplant Recovery
The procedure itself is only half the story. Recovery discomfort is real but predictable, and it follows a consistent pattern. Days 1 through 3 are the peak discomfort window, with most patients describing a sunburn-like tightness across the donor area and mild throbbing in the recipient zone. By day 5, the majority of patients report minimal pain without medication.
Post-Operative Care and Medication
A standard post-operative pain management protocol includes:
- Oral analgesics: Paracetamol (1,000mg every 6 hours) or ibuprofen (400mg every 8 hours) for the first 3 to 5 days
- Prescribed medication: Some surgeons provide a short course of tramadol or codeine for patients with lower pain thresholds
- Anti-inflammatory sprays: Saline solution applied to the recipient area every 2 hours during the first 48 hours reduces swelling and irritation
- Sleep positioning: Sleeping at a 45-degree angle on a travel pillow for the first 5 nights minimizes swelling and pressure on grafts
- Cold compresses: Applied to the forehead (never directly on grafts) for 15-minute intervals to reduce frontal swelling that peaks around day 3 to 4
Avoid alcohol, blood thinners, and strenuous exercise for at least 10 days. These increase blood flow to the scalp and can intensify throbbing sensations. Most patients return to desk-based work within 2 to 3 days and resume full physical activity by week 3.
Long-Term Comfort and Final Results Expectations
Temporary numbness in the donor area can persist for 4 to 8 weeks as nerve endings regenerate. This is normal and resolves without intervention. Occasional tingling or itching in the recipient zone between weeks 2 and 6 signals healthy healing and new follicle activity.
The transplanted hairs enter a shedding phase (shock loss) between weeks 2 and 4, which causes no pain. New growth becomes visible around month 3 to 4, with significant density appearing by month 8. Final results are typically assessed at 12 to 14 months. Track your progress by taking monthly photos under consistent lighting, focusing on the hairline and crown from the same angles each time. This gives you an objective record of density improvement that is far more reliable than daily mirror checks.
The fear of pain should not prevent anyone from restoring their hair. Modern anaesthesia techniques, needle-free injection systems, and structured recovery protocols have made the experience manageable for the vast majority of patients. Choose a clinic with a transparent anaesthesia protocol, ask specifically about their pain management approach during your consultation, and you will find the reality far easier than the anticipation.
FAQ
Most clinics prescribe paracetamol or ibuprofen for 3 to 5 days. Stronger options like tramadol may be provided for patients with higher sensitivity. Anti-inflammatory sprays and cold compresses supplement oral medication.
Expect a sunburn-like tightness for 2 to 3 days, rated 2 to 4 out of 10 by most FUE patients. FUT patients may experience slightly higher soreness around the suture site for up to 10 days.
Yes, for most patients. The initial needle pricks last about 5 to 10 minutes and are the peak discomfort moment. Needle-free systems reduce this significantly, and once numbness sets in, the rest of the procedure is painless.
Local anaesthesia with lidocaine and epinephrine is the standard. Topical numbing cream is often applied beforehand, and some clinics use needle-free delivery systems for the injections themselves.
The procedure causes minimal pain once anaesthesia takes effect. Most patients rate the experience as far less uncomfortable than expected. Recovery discomfort is mild and well-controlled with standard over-the-counter medication.